 Surgery is a commonly used treatment option for patients with laryngeal cancer. However, the effectiveness of this option depends also on proper surgical documentation. Though there are different surgical operations used to remove the cancer (for example, laser surgery, laryngectomy, cordectomy), otolaryngologists recommend procedures depending on the stage and location of the cancer. Unless the patients’ medical reports contain details about the development of laryngeal cancer, surgeons can’t determine which surgical procedure will be appropriate for their patients and the wrong choice will adversely affect the patients’ health.
Surgery is a commonly used treatment option for patients with laryngeal cancer. However, the effectiveness of this option depends also on proper surgical documentation. Though there are different surgical operations used to remove the cancer (for example, laser surgery, laryngectomy, cordectomy), otolaryngologists recommend procedures depending on the stage and location of the cancer. Unless the patients’ medical reports contain details about the development of laryngeal cancer, surgeons can’t determine which surgical procedure will be appropriate for their patients and the wrong choice will adversely affect the patients’ health.
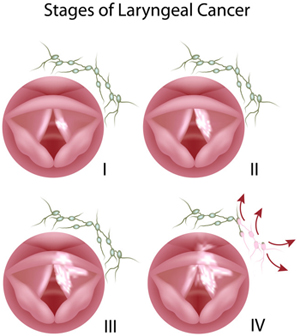
A study published in the August issue of JAMA Network Journal says that surgical therapy leads to better survival rates with the patients having advanced (Stage III or IV) laryngeal cancer compared to non-surgical therapy (for example, chemoradiation). It was found the patients who had surgery had 2-year and 5-year disease-specific survival and 2-year and 5-year overall survival compared to patients who did not undergo surgery. Now, the challenge is how to determine whether it is advanced laryngeal cancer. Prognosis of laryngeal cancer is always associated with the size and site of the lesion and hence the documentation of size and site of the lesion is very important for determining advanced cancer. Unless the exact anatomic site and size of cancer is properly documented, otolaryngologists can’t determine how severe the cancer is and whether surgery will be an effective option. If the cancer is in its very early stage, preventive measures or chemoradiation may be effective.
The risks and side effects associated with the surgery is a major issue. Patients who had a laryngectomy typically lose their ability to speak normally and it can also lead to the development of a fistula, which may require another surgery. Surgeries affecting the throat or voice box may result in gradual narrowing of the throat or larynx (if it retains after surgery), which could affect breathing in some cases. Larynx surgeries may also affect the patients’ ability to swallow in certain cases which will affect how they eat and may require a permanent feeding tube in some cases. Detailed documentation of treatment and follow up of patients who have undergone surgery is quite important to address these issues. Surgeons can then understand the exact problems patients have from their medical documents and take efforts to find the right solutions. They can check the patients’ response to the solutions and look for opportunities of improvement.
Electronic Health Records (EHRs) provide you with standardized documentation that will help enhance communication between patients and physicians as well as between family practice physicians and surgeons. This will also enable surgeons to find out more about the cancer development and decide whether surgery will be effective. The automated data entry method will improve the speed of decision making. Surgeons can also access the treatment details and recommend remedies quickly. However, the major disadvantages with this system are:
- Physicians may copy and paste data within EHR vigorously to save time and this may result in missing information, duplication or other data errors which will lead to erroneous data in EHR fields. If the information in the EHR fields happens to be incorrect, it will be quickly transferred to other parts of the system as it may autopopulate fields with the data derived from a prior report.
- The use of drop-down menus, point-and-click lists, autofill, templates, and canned text within the electronic system can produce redundant and formulaic information so that significant clinical information may remain unnoticed.
The best alternative is the combined use of EHR and transcription. Professional transcriptionists can transcribe physicians’ and surgeons’ dictations and enter the transcribed content into the appropriate fields through the use of Discrete Reportable Transcription (DRT) technology. Efficiency and accuracy of the documentation can be ensured at the same time with this system.


