Table of Contents
Healthcare providers have a lot on their plates between tending to patients, offering advice, and performing regular checkups. They also have to maintain accurate patient records and documentation, which can be difficult to accomplish. To make their jobs easier, medical professionals such as physicians, nurses, and nurse practitioners use voice recorders to capture their notes. Medical transcription is then used to transcribe the notes. Reliable medical transcription companies assist doctors in creating accurate medical records. With such professional assistance, healthcare providers can focus on giving their patients the best care possible.
Significance of Medical Records and Treatment Planning
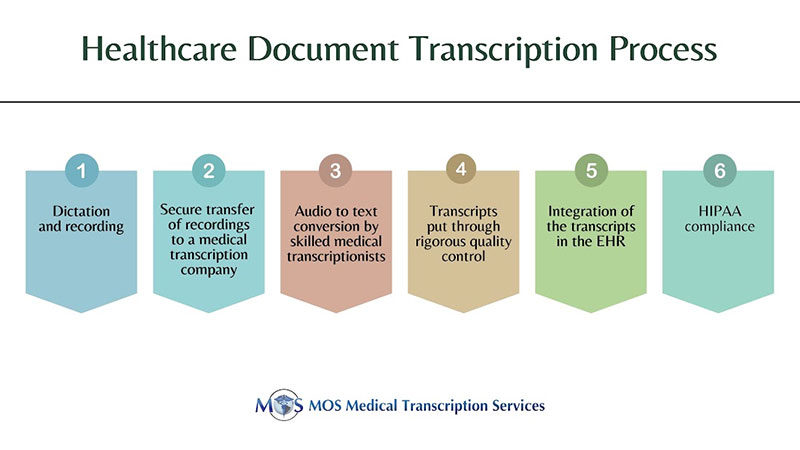
Doctors record detailed information about their patients’ health, including lab and pathology results, prescribed medications, past and present illnesses, tests, and diagnoses in the form of audio recordings. A medical transcriptionist listens to the audio recording, transcribes it into text format, and then ensures there are no errors or inconsistencies. A reliable medical transcription company will have state-of-the-art quality assurance procedures in place to ensure accuracy in the medical documentation. This record is now part of the patient’s medical history and can be viewed by physicians, nurses, and other healthcare professionals as needed.
Accurate medical records are important for developing a good treatment plan. A treatment plan is a documented approach to managing a patient’s disease or damage which often includes details about the ailment, the precise goals of the treatment, every option for achieving those goals (together with any potential side effects and other pertinent factors), and expectations on the course and length of the treatment. In order for patients and healthcare providers to comprehend and treat any health problem, treatment plans are crucial.

Role of Medical Transcription in Treatment Planning
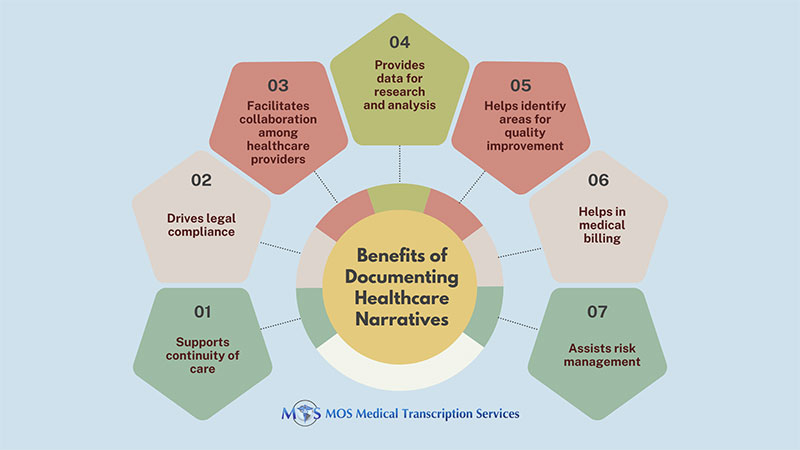
- Accurate patient records: Precise documentation is vital throughout the treatment planning process, from the first diagnosis to long-term care. Medical transcriptionists act as guardians, making sure that the data recorded by medical practitioners is accurate, clear, and devoid of any ambiguity. This data includes important information such as test results, prescriptions, directions for follow-up, and any other relevant data. Medical transcriptionists play a crucial role in enabling healthcare providers to make well-informed treatment plans by providing accurate and comprehensive patient records.
- Legal and ethical compliance: Beyond accuracy, maintaining legal and ethical standards in healthcare is important. Patient record documentation should comply with rules and regulations, just as every other aspect of healthcare. Medical transcriptionists follow these rules and regulations to guarantee accurate records and protect patient confidentiality. Healthcare practitioners can better adhere to legal requirements and privacy standards, including the Health Insurance Portability and Accountability Act (HIPAA), with the support of experienced and dedicated medical transcription services.
- Coordination and communication: Medical transcription plays a crucial role in treatment planning as well because it serves as a bridge for professional healthcare communication and collaboration. The essential data that different members of a healthcare team need to effectively collaborate is captured in the transcribed records. Precise documentation facilitates easy access to a patient’s medical history, progress, and treatment plans, leading to improved coordination and communication. This aspect becomes particularly important when a patient receives care from different providers. Accurate transcripts of various medical encounters and treatments provided support the continuum of care and prevent treatment gaps or errors. Effective collaboration and communication are the cornerstones of a successful treatment strategy. Medical staff must coordinate their efforts in the direction of a common goal, providing patients with the best possible treatment plan. Medical transcriptionists help in this attempt by providing thorough and detailed records that act as a communication channel between members of the healthcare team.
- Make better clinical decisions: Medical professionals depend on clinical documents for the insights they provide into a patient’s past medical history, current health, and reaction to previous therapies. Additionally, medical records serve as a compass for decisions about diagnosis and treatment. Test findings and medication histories act as road signs that point doctors in the direction of the most prudent course of care. To guarantee the continuity of care, doctors may also consult previous notes and follow-up recommendations. To make well-informed judgments about patient care, diagnosis, and treatment options, healthcare professionals refer to comprehensive patient histories, test results, and treatment plans. Accurate and comprehensive medical records, made possible through medical transcription, play a pivotal role in clinical decision-making.
- Billing and Insurance: Precise and comprehensive transcripts hold great importance in insurance billing and claims procedures. These documents are what insurance companies use to verify the legitimacy and need of medical treatments provided to patients. Incomplete or inaccurate paperwork may result in delays, claim denials, or even legal complications. Careful documentation is essential to guarantee that healthcare practitioners are fairly and promptly compensated for their services. Additionally, it benefits patients by preventing inaccurate paperwork that might result in erroneous charges and unforeseen out-of-pocket costs.
Medical Transcription Services Can Ensure Accurate Medical Documentation
Medical transcription is thus an important part of improving the standard of patient care. Due to advancements in technology, strict adherence to regulations, and the critical components of prompt transcriptions and clear communication, the process has transformed into an increasingly accurate and efficient undertaking. Medical transcription services providers focus on generating accurate medical records, which are vital from the viewpoint of patient care delivery and administrative workload efficiency.